2. Treatment
Treatment
Digital health technologies have the potential to change therapeutic methods and improve clinical outcomes.
In this “therapeutic” context they are called “Digital Therapeutics (DTx)”. The precise definition of a digital therapeutic is still up for some debate and variations exist; the Digital Therapeutic Alliance (https://dtxalliance.org/understanding-dtx) offers the following descriptive definition:
“Digital therapeutics (DTx) deliver evidence-based therapeutic interventions that are driven by high quality software programmes to prevent, manage, or treat a medical disorder or disease. They are used independently or in concert with medications, devices, or other therapies to optimise patient care and health outcomes.
DTx products incorporate advanced technology best practices relating to design, clinical evaluation, usability, and data security. They are reviewed and cleared or certified by regulatory bodies as required to support product claims regarding risk, efficacy, and intended use. The Alliance in addition stipulates a set of foundational principles for DTx (see box)
All products claiming to be a digital therapeutic must adhere to these foundational principles:
|
Examples
Digital therapeutics can be used in combination with existing medications or as standalone agents:
1. DTx can be used concurrently with existing medication to optimise the dose/consumption or improve medication adherence. In 2017, FDA approved the first medication that contains a sensor (ABILIFY MYCITE®). The sensor will be activated after consumption of the pill by the patient and submit the patient’s activity and sleep reports to a smartphone. Patients can also report their mood and general condition. More information about the smart pill system is available in this video:
2020 Otsuka America Pharmaceuticals Inc.April 2020 12US20EBC0029
This example shows how a combination of medication and a sensor enables clinicians to optimise the dose and interval of taking medication and eventually minimise the risk of adverse events and maximise the clinical benefit. Poor medication adherence is another challenge, especially for chronic non-communicable diseases, that can be addressed with DTx. It increases morbidity and mortality rates, resulting in costs of $528.4 billion annually [1]. Digital health solutions can improve medication adherence using, for example, nudging1, gamification2 and cognitive behavioural therapy (CBT3) techniques.
2. DTx can be designed to function as a standalone therapeutic agent and improve clinical outcomes. It provides therapeutic value in conditions such as substance use disorder (SUD), sleep disorders, phobia, usually through cognitive behavioural therapy (CBT) (Table 1).
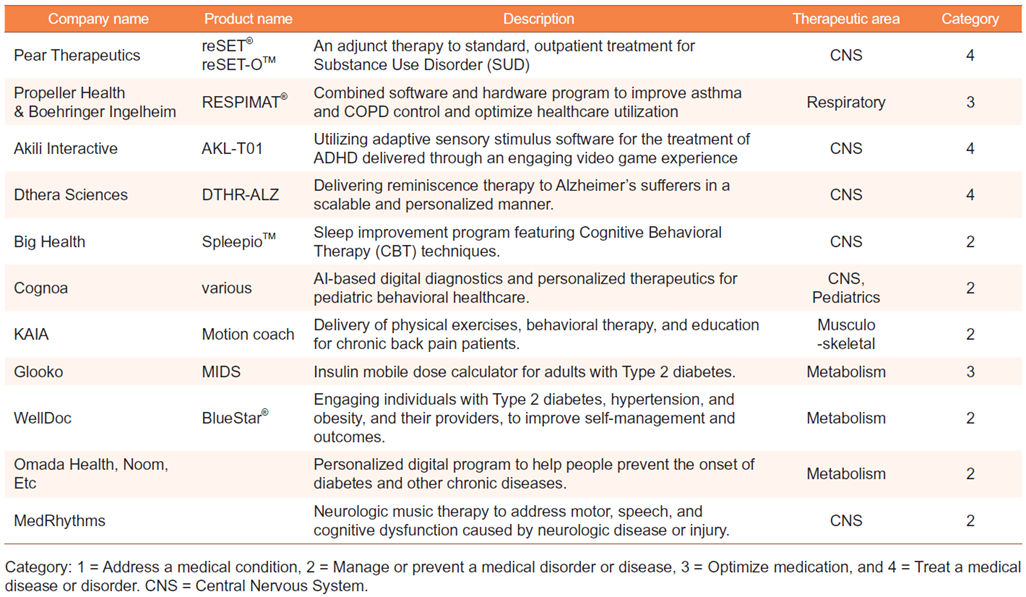
Table 1: Examples of Digital Therapeutics under development or on the market [2]
Note 1: Nudging: First-generation digital therapeutic solutions did groundbreaking work around behavior change, using an important concept known as the nudge. A nudge is a prompt or a reminder, designed to elicit beneficial behavior. A nudge is not a command: the person being nudged can always decide to take the recommended action or not. While the application of personalized nudges was a breakthrough in digital health, behavioral science offers many additional approaches to personalization that can lead to better outcomes for more people. Using data analytics, artificial intelligence, and psychological research, digital health providers like DarioHealth continue to optimize personalization for every individual. https://www.dariohealth.com/articles/digital-health-beyond-the-nudge/
Note 2: Gamification refers to leveraging mechanics and other experiential elements typically associated with games in non-game contexts. These can be fairly subtle (e.g. a progress bar for filing out a health risk questionnaire), moderate (e.g. achievements given for reaching personal finance goals, contests for steps walked as a team in a workplace wellness competition), or extreme (e.g. an augmented reality experience to treat chronic pain).
Note 3: Behavioural science has shown that individual decision-making is highly linked to emotions and beliefs. Therefore, an app that aims to create sustainable behaviour change needs to provide a positive emotional experience. An app that targets the brain by delivering motivational stimuli relating to core beliefs can influence individual behaviour and decision-making. Over time, every user builds a personal digital footprint that allows the DTx to provide more personalised nudges, leading to personalised engagement. https://sidekickhealth.com/news/clinically-proven-dtx-improve-wellbeing/
References
[1] Klein D. Medication Non-Adherence: A Common and Costly Problem.; 2020
[2] Chung JY. Digital therapeutics and clinical pharmacology. Translational and Clinical Pharmacology. 2019;27(1):6. doi:10.12793/TCP.2019.27.1.6