Semi-synthetic Chemical Medicines
| Site: | EUPATI Open Classroom |
| Course: | Types of Medicines and Their Mode of Action and Use |
| Book: | Semi-synthetic Chemical Medicines |
| Printed by: | Guest user |
| Date: | Tuesday, 8 July 2025, 9:54 AM |
1. General features
Semi-synthetic medicines are derived from natural products, which often provide a useful starting point for the discovery of physiologically effective molecules and therefore play an important role in the development of new medicines.Both fully synthetic and fully natural compounds have some limitations that can be overcome by using a semi-synthetic alternative. Many naturally occurring molecules could potentially be used as medicines but may not be effective because they are chemically
unstable, not easily absorbed by the human body or induce unwanted side effects. Potentially useful fully synthetic molecules may also fail as medicines for the same reasons. In addition, fully synthetic molecules are technically challenging to create
‘from scratch’ in the laboratory, particularly if scientists do not know the precise details of how they bind to target cells to achieve their effects.
Modification of a natural product can therefore be a useful alternative when fully synthetic compounds would be too complex or expensive to produce, and the natural product alone does not meet all the criteria of a useful medicine. The modifications made
to natural compounds can improve factors such as chemical stability
or solubility
in water, and the strength of interaction between a medicine and the cells that it binds to in the body.
Like chemical medicines, semi-synthetic medicines are relatively small and simple molecules compared with biologic medicines (see section on biologics), which may contain proteins such as enzymes and antibodies.
2. Mode of action
Semi-synthetic medicines work in the same way as chemical medicines (see the section on chemical medicines) – they only differ in their mode of production, not in their mode of action.3. Production process
In principle, the chemical production of semi-synthetic medicines is identical to that of fully synthetic medicines (see section on chemical medicines), although the starting point is different. Unlike fully synthetic medicines, which are created entirely in the laboratory using a stepwise combination of small chemical building blocks, semi-synthetic medicines are derived from naturally occurring substances extracted from sources such as plants, bacteria or animal cells.The first step in isolating natural molecules from living tissue is a process called extraction; for example, to extract biomolecules from plants, leaf or root tissue may need to be washed, freeze-dried and ground to produce a clean and uniform sample. Also, the biomolecule may be isolated from a fermentation broth from, for example, genetically modified microorganisms. The sample is then purified to isolate the active ingredient by further steps, which may include filtration or the use of solvents such as ethanol (alcohol).
After extraction and purification, the isolated molecule can then be modified using standard laboratory techniques, for example by incorporating additional molecules such as phosphate or alcohol. This modification takes place in specialised factories under quality-controlled conditions.
4. Mode of administration
Semi-synthetic medicines are taken in the same way as other medicines, most commonly as tablets, creams, sprays or injections.5. Example - Antibiotics
Antibiotics (also known as antibacterial) are used to treat or prevent disease caused by bacteria or certain parasites, such as infections of the lungs or the skin. They kill bacteria or prevent them from multiplying by targeting their growth and reproduction. Alexander Fleming (1881-1955) discovered the first modern-day antibiotic in 1928 when he noticed that a mould had killed some bacteria that he was growing in his laboratory. The active ingredient of the mould that Fleming discovered, penicillin, was isolated and quickly became apparent that the naturally occurring form of the molecule had a narrow range of action, and was rapidly broken down by bacterial enzymes. It has, since then, been modified to improve its stability and efficacy for use as an antibiotic medicine. Using a semi-synthetic approach, the chemical structure of natural penicillin was modified. The introduction of penicillin and other antibiotics in the 1930s and 1940s was one of the most important breakthroughs in medicine.
Today, doctors have access to hundreds of different antibiotics, such as ampicillin, amoxicillin, erythromycin and tetracycline, which can be taken using a number of methods, such as orally as tablets, applied externally as topical creams or eye drops, or injected directly into muscles or veins.

Figure 3.1. Alexander Fleming (https://en.wikipedia.org/wiki/Alexander_Fleming)
It is essential to take the complete prescribed course of antibiotics. Bacteria can become resistant to certain antibiotics, particularly if they are exposed to a low dose. They do this so quickly that there is a constant need for research to keep side by side of the changes occurring. A well-known example of this is MRSA (methicillin-resistant Staphylococcus aureus), a species of bacteria that has acquired resistance to a wide range of different antibiotics. MRSA infections are very difficult to treat and can be life-threatening. Antibiotics – which kill living bacteria – are ineffective against viral infections (such as influenza or ‘flu’). To read more about this issue see IMI New Drugs for Bad Bugs ND4BB (http://www.imi.europa.eu/content/nd4bb).
Importantly, some people are allergic to penicillin and similar antibiotics, and in rare cases allergic reactions can be severe, and even result in death.
6. Example - Steroids
Steroid hormones are naturally produced in the human body and are important in many physiological processes such as the stress response, inflammation and immune responses, and reproduction. Naturally occurring hormones can be modified to create medicines for pharmaceutical use. For example, glucocorticoids are semi-synthetically created from the natural hormone cortisol. Glucocorticoids are prescribed as medicines to treat a range of inflammatory conditions including joint pain and arthritis , asthma and allergic reactions.Another example is ethinyl estradiol, which is made by semi-synthetic processing of the naturally occurring hormone estrone (an estrogen hormone) and is commonly used in contraceptive pills.
Cortisol and oestrone were originally isolated from animals (cortisol was extracted from the adrenal glands of pigs and cows, and oestrone was purified from the urine of pregnant horses), but they are now both produced in the laboratory by genetically modified microorganisms, such as yeast.
7. Example - Anti-cancer medicines
Cancer is often treated with chemotherapy medicines that kill cells undergoing rapid growth (which most cancer cells do). One example of a semi-synthetically derived anti-cancer medicine is irinotecan, which is mainly used to treat colon cancer.

Figure 1.2 Camptotheca acuminata (Link to the source)
Irinotecan is produced by chemical modification of camptothecin, a molecule naturally produced by Camptotheca acuminata, called the ‘happy tree’ that is native to China. When researchers discovered camptothecin and tested its potential as a cancer medicine, they observed anti-tumour activity – but also found that the treatment induced unpredictable side effects. Consequently, camptothecin was chemically modified to develop the new medicine irinotecan, which has a more predictable side-effect profile than the naturally occurring molecule. The synthesis of irinotecan from camptothecin requires extensive modification of the chemical structure (Figure 3.3).
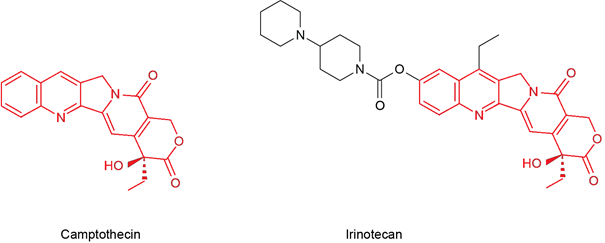
Figure 3.3. Chemical structure of naturally occurring camptothecin and the semi-synthetic irinotecan.
8. Example - Anti-malarial medicines
Malaria is an infectious disease caused by a parasite, such as the parasitic microorganism Plasmodium, which is transmitted to humans through mosquito bites. Patients with malaria initially experience relatively mild flu-like symptoms, but the disease can rapidly become life-threatening and cause breathing problems or organ failure.
Figure 3.4 Artemisia annua (source here)
The plant sweet woodworm (Artemisia annua) has been used in traditional Chinese medicine for thousands of years to treat infections with Plasmodium. The medicinally active chemical component of sweet woodworm is called artemisinin, and was successfully isolated in 1972. Since then, semi-synthetic production of artemisinin has considerably improved its pharmaceutical properties, and derivatives of artemisinin are now commonly used as anti-malarial medicines throughout the world.